At Operation Fistula, we are all too familiar with the injustices experienced by women living with obstetric fistula. Despite the existence of a dedicated community of fistula surgeons and a surgical treatment viewed by many as successful in alleviating or eliminating symptoms (1), the pace of obstetric fistula continues to outrun our collective ability to treat it. The need to address prevention and treatment efforts has been urgent for some time, but with the COVID-19 pandemic and its myriad consequences, the need has become acute.
Operation Fistula has a legacy of developing innovative solutions to the most pressing issues around obstetric fistula. During our Pilot Program (2012-2015), we pioneered a performance-based funding scheme that increased surgical throughput by 39%. We dedicated several years to developing the tools and technology necessary for verifying and measuring our work; GOFAR continues to be a hallmark feature in our programs around the world. In the past year, we focused on the patient journey and improving methods for patient identification, mobilization, and treatment. Through it all, we heard the same issue raised by surgeons again and again: they needed funding to perform fistula repairs.
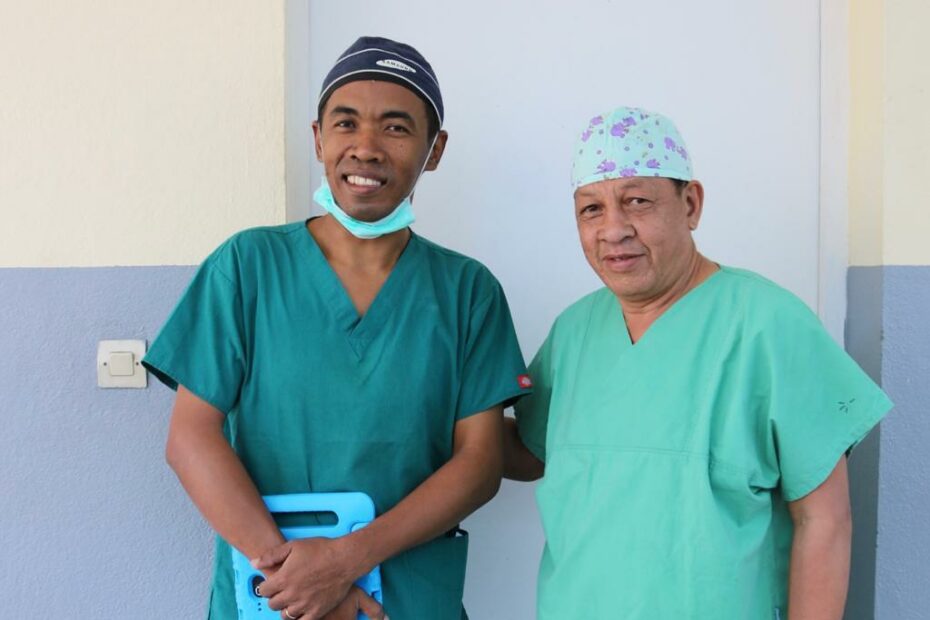
The surgeons we partner with have access to the newest technology and approaches to finding and treating patients, but without funding, none of it matters. We know surgeons who have funded patient care from their own pockets; every surgery they can’t afford to perform is a fistula patient whose life continues to be devastated by fistula. A lack of accessible funding for fistula surgeons severely limits their capacity to treat and care for patients. This is the problem we seek to solve with Kickstart – our new and improved funding program, going live this month.
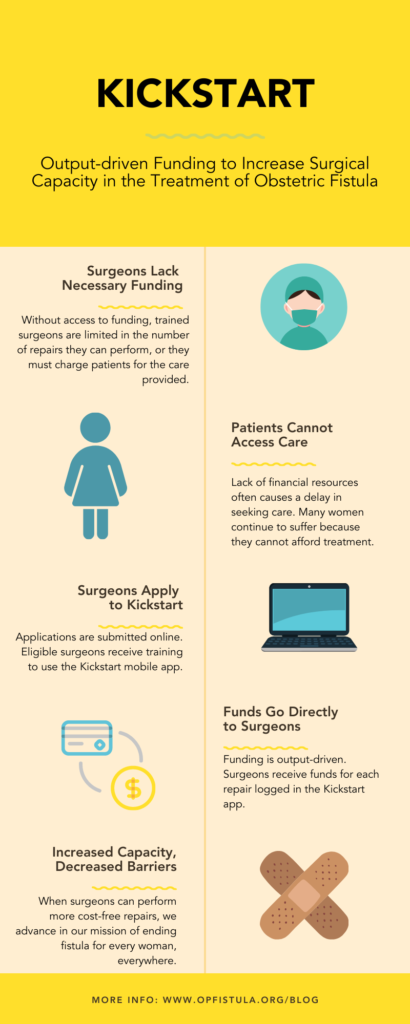
OUTPUT-DRIVEN FUNDING TO INCREASE CAPACITY
Kickstart is an output-driven funding program that provides funds directly to surgeons for each repair they perform and record using our data collection technology – GOFAR. As its name implies, the program is meant to ‘kickstart’ or catalyze the abilities of surgeons to treat fistula patients, by removing the financial barriers that previously limited their capacity.
Kickstart is directed at trained surgeons who are limited in the number of repairs they can perform because of a lack of funding. For each surgery logged in GOFAR, we provide funds directly to the surgeon. The data entered by the surgeons helps us track and monitor their performance, and also feeds a centralized data repository. Operation Fistula analyzes all this data, to evaluate programmatic indicators in real-time, and identify trends or patterns in fistula treatment. All the surgeries funded through Kickstart are performed at no cost to the patient, which given the resource constraints faced by these surgeons, would have otherwise been impossible.
We believe in the power of proximity, and have always championed innovation and advocated for solutions that come from those working closest to the problem. In October, we sent out the first wave of Kickstart applications to surgeons. In their responses, nearly every surgeon who applied to participate, reported that external funding for treatment expenses was a significant barrier to providing care. If they are not working at a facility where fistula care is funded by a larger organization, surgeons may have no option but to charge patients. We know from our outreach work that patients fear the cost of treatment, and this prevents them from seeking care. Many obstetric fistula patients lack even the funds necessary for transport to the facility, so any cost represents a major barrier. When surgeons are put in a position where they are forced to charge patients for their care because they have no other funding available to them, it discourages patients from seeking care and perpetuates their distrust of healthcare systems and providers.
Funding barriers have contributed to the ever growing backlog of patients; the number of surgeons that are able to perform fistula repairs simply cannot keep up with the demand for treatment. The World Health Organization estimates that between 50,000-100,000 people develop obstetric fistula each year (2). Without immediate intervention to increase surgical capacity, this list of patients awaiting treatment will continue to grow.

Catalyzing Capacity and Care
Kickstart complements our ongoing mission to end fistula for every woman, everywhere. With this program, we are renewing our commitment to ensuring that patients receive the treatment they urgently need, and surgeons have the capacity necessary to provide that care. In providing output-driven funding, Operation Fistula is increasing the capacity of existing surgeons to perform more repairs, and removing the financial barrier to treatment that is frequently cited by fistula patients (3).
Applications to join the Kickstart program and receive output-driven funding are now open. To submit an application in English, please complete this online form. If you would prefer to complete the application in French, an alternative form is available here. For any questions related to Kickstart, please do not hesitate to contact Operation Fistula via email at kickstart@opfistula.org.
Citations
- Rupley, MD DM, Dongarwar, MS D, Salihu, MD, PhD HM, Janda, MD AM, Pope, MD, MPH R. Healthcare Access as a Risk-Marker for Obstetric Vesicovaginal Fistula in Malawi. International Journal of Maternal and Child Health and AIDS. 2020;9(1):4–13.
- WHO. The Second Meeting of the Working Group for the Prevention & Treatment of Obstetric Fistula. Addis Ababa; 2002 Nov.
- Baker Z, Bellows B, Bach R, Warren Charlotte. Barriers to obstetric fistula treatment in low‐income countries: a systematic review. Tropical Medicine & International Health. 2017 Aug;22(8):938–59.